Nutrition
Contents
1 Fat
Fats typically consist of fatty acids (long chains of carbon and hydrogen atoms with a carboxyl group at one end) bonded to a "backbone" such as glycerol.
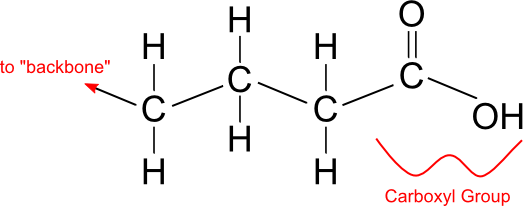
Fatty Acid

Glycerol "backbone"
When metabolised, fats are broken down into glycerol and free fatty acids.
1.1 Saturated Fats
If every carbon atom in a fatty acid chain is bonded to two hydrogen atoms, as in the figure above, then it is called saturated. The carbon atoms are saturated with hydrogen, which means they are bonded to as many hydrogens as possible.
1.2 Unsaturated Fats
If a carbon atom in a fatty acid chain is bonded to only one hydrogen atom, and instead of being bonded to a second hydrogen atom is double-bonded to a neighbouring carbon atom, then the fatty acid is called unsaturated. A fatty acid with only one double bond is called monounsaturated whereas a fatty acid with multiple double bonds is called polyunsaturated.
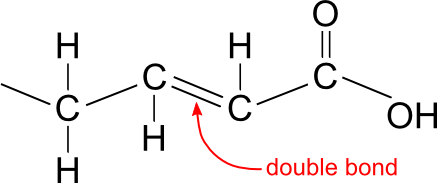
Unsaturated fatty acid
1.3 Trans and Cis Fats
In an unsaturated fatty acid, there are two ways in which a double bond might be arranged. If both parts of the chain appear on the same side of the double bond then it is called a cis-isomer. If one part of the chain appears on one side of the double bond and the other on the opposite side then it is called a trans-isomer. Fats containing trans-isomer fatty acids are commonly called trans fats.
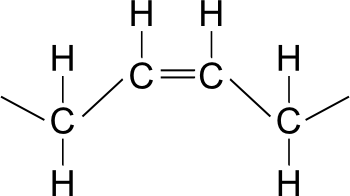
Cis-isomer fatty acid
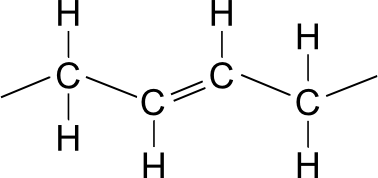
Trans-isomer fatty acid
A cis-isomer double bond introduces a "kink" into the chain, which prevents the fatty acid chains from packing together tightly. Among other things, this lowers the melting point of cis-isomer fats so that they tend to be liquid at room temperature. In contrast, trans fats can pack tightly together to form a solid that is harder to break apart and thus has a higher melting point.
1.4 Nutritional Functions of Fat
1.4.1 Fuel
Fats are a very good source of energy: they provide about 9 calories (37.8kJ) of energy per gram [1].
1.4.2 Vitamin Bearing
Vitamins A, D, E and K are fat-soluble. This means that they can only be digested, absorbed and transported in conjunction with fats. A decrease in absorption of fat may result in a decrease in absorption of these vitamins [2].
1.4.3 Essential Fatty Acids
Certain fatty acids are required for various biological functions besides just acting as a fuel source. Of those fatty acids, some can be synthesised by the human body from other food components and some cannot. Those that the human body cannot synthesise, and which therefore must be ingested, are called essential fatty acids (EFAs) [3].
EFAs are unsaturated fatty acids. The carbon atom at the end of the fatty acid chain next to the carboxyl group is known as α (alpha). The carbon atom at the other end of the chain is known as ω (omega). The physiological properties of EFAs are largely dependent on the position of the first double bond relative to ω. They are therefore classed according to the position of that double bond. For example, if we move along the chain from ω, counting carbon-to-carbon bonds as we go, and we find 5 single bonds and then the 6th bond is a double bond, then this fatty acid is an ω-6 fatty acid.
Within each class of fatty acid, different molecules are further specified by counting the number of carbon atoms in the chain and the number of double bonds within the chain. Consecutive double bonds are assumed to be separated by a single carbon atom unless otherwise specified. For example, stearidonic acid has a chain of 18 carbon atoms with 4 double bonds, the first of which is the third bond from the ω end of the chain. It is therefore written like this: ω-3 18:4.

stearidonic acid
There are only two EFAs:
- α-linolenic acid (αLNA) ω-3 18:3
- linoleic acid (LA) ω-6 18:2
However, there are a number of other fatty acids which perform vital biological functions and are therefore sometimes referred to as EFAs, even though strictly speaking they are not "essential" since the human body can synthesise them from αLNA or LA [4].
- eicosapentaenoic acid (EPA) ω-3 20:5
- docosahexaenoic acid (DHA) ω-3 22:6
- γ-linolenic acid (γLNA) ω-6 18:3
- dihomo-γ-linolenic acid (DγLNA) ω-6 20:3
- arachidonic acid (AA) ω-6 20:4
The ease and efficiency with which these fatty acids can be synthesised from αLNA or LA determines how likely they are to be considered "essential".
EFAs appear to be important for a whole host of different biological functions.
ω-3 fatty acids are currently being investigated as preventative agents in coronary heart disease, diabetes, thyrotoxicosis, bronchial asthma, multiple sclerosis and psoriasis, primarily as a result of a study comparing the health and diets of the inhabitants of Greenland with mainland Danes [5].
Increasing the relative proportions of ω-3 fatty acids ingested compared to ω-6 fatty acids seems to moderate inflammatory reactions, which are "at the basis of a number of disease processes in virtually any systemic or organ-specific disease, ranging from classical rheumatic diseases to bronchial airway hyper-responsiveness, inflammatory bowel disease, kidney diseases, psoriasis and atopic eczema" [4]. Most of these diseases appear to share a background in inflammation or derangement of immune systems.
EFAs, especially arachidonic acid, are also involved in neurological processes. "The arachidonic acid cascade is arguably the most elaborate signaling system neurobiologists have to deal with" [6]. AA appears to be related to various mental conditions, including bipolar disorder and Alzheimer disease [7].
1.5 Health Concerns
1.5.1 Saturated vs. Unsaturated
Although a lot of people, including the World Health Organisation, the United States Centers for Disease Control, the American Heart Association, the UK Food Standards Agency, and loads of others, recommend minimising the amount of saturated fat in your diet, I cannot actually find any particularly good reason to do so. They all seem to claim that saturated fats cause cardiovascular disease but I don't know why they say that.
So far, I have only found two meta-analyses of research into possible links between saturated fat and cardiovascular diseases [8] [9], both of which conclude that there is no statistically significant link.
The UK Food Standards Agency claims that "Eating a diet that is high in saturated fat can raise the level of cholesterol in your blood, over time. This increases your chance of developing heart disease" [10]. But they don't cite any evidence to back up that claim.
A study of two populations of Polynesians seems to support the theory that an increased level of dietary saturated fat causes an increase in cholesterol levels: "Tokelauans obtain a much higher percentage of energy from coconut than the Pukapukans, 63% compared to 34%, so their intake of saturated fat is higher. The serum cholesterol levels are 35 to 40 mg higher in Tokelauans than in Pukapukans. These major differences in serum cholesterol levels are considered to be due to the higher saturated fat intake of the Tokelauans." However: "Vascular disease is uncommon in both populations and there is no evidence of the high saturated fat intake having a harmful effect in these populations" [11].
In post-menopausal women, a diet high in saturated fat is associated with less progression of coronary atherosclerosis, whereas replacing other fats with polyunsaturated fat is associated with greater progression (monounsaturated fats and total fat intake are not associated with progression at all) [12].
Heating polyunsaturated fats (e.g. when using them for frying or other forms of cooking) may cause them to break down into toxic chemicals and trans fats [13].
1.5.2 Trans Fats
In contrast to the saturated/unsaturated confusion, everyone seems to agree that trans fats are very bad for you. There does appear to be a strong statistical link between the consumption of trans fats and cardiovascular disease [14].
One proposed mechanism for the causation of cardiovascular disease by trans fats is the observation that trans fats raise the level of low-density-lipoprotein (LDL) cholesterol in the blood while simultaneously lowering the level of high-density-lipoprotein (HDL) cholesterol.
Lipoproteins are the complex molecules that transport cholesterol through blood. The density of a lipoprotein refers to the ratio of cholesterol to protein within the molecule: the more cholesterol and the less protein it has, the less dense it is. LDL cholesterol is positively correlated with cardiovascular disease and diabetes, whereas HDL is negatively correlated with those diseases [15]. Thus simultaneously raising LDL while lowering HDL would seem to be the worst of both worlds.
(Incidentally, perhaps a failure to distinguish between different lipoprotein densities is behind the apparently unjustified condemnation of saturated fats?)
Trans fats also appear to inhibit the enzymatic desaturation of linoleic and α-linolenic acids, thus preventing the synthesis of important essential fatty acids [14]. As noted above, EFAs are linked to the prevention of coronary heart disease, so the prevention of their synthesis is evidently not a good thing.
Trans fats only occur in trace amounts in nature. They do not occur in plant matter at all and only occur in very small amounts in meat from ruminants (such as cattle and sheep) [16]. Almost all the trans fat consumed by humans today is created by the process of partial hydrogenation. This process begins with a natural unsaturated fat (which will always be a cis-isomer) and then modifies the fatty acid chains in order to saturate some of the unsaturated double bonds. However, the hydrogenation is only partial: some double bonds remain and some of those that do remain are transformed from cis-isomer bonds to trans-isomer bonds. This process is popular in the food industry because it turns fats that are liquid at room temperature into solids, which are more convenient for storage (they are less susceptible to turning rancid and so have a longer shelf-life and require less refridgeration) and can be used as low-cost replacements for the solid fats used in baking. The use of margarine to replace butter or lard is a good example of this. Trans fats are also used for deep-frying in restaurants as they can be used for longer than natural oils before they turn rancid. They are therefore very popular in the fast food industry.
So not only are trans fats very bad for your health in themselves but they are also used to replace natural fats and so reduce your consumption of essential fatty acids.
1.5.3 Essential Fatty Acids
As noted above, EFAs are vital for a wide range of biological processes. Although only two fatty acids are strictly "essential", i.e. impossible for the human body to synthesise, the ability to synthesise the other important fatty acids, especially EPA and DHA, is limited:
Two main families of long-chain polyunsaturated fatty acids exist, biologically derived from the shortest non-synthesizable precursors linoleic acid (C18:2n-6) and alpha-linolenic acid (C18:3). Linoleic acid is abundant in oils from most vegetable seeds such as corn and safflower. Alpha-linolenic acid is found in the chloroplasts of green leafy vegetables. Humans can desaturate and elongate alpha-linolenic acid to eicosapentaenoic acid (EPA) and, further, to docosahexaenoic acid (DHA). However, the elongation and desaturation processes are likely to be slow and possibly further limited with ageing and disease conditions. For these reasons, EPA and DHA are considered, to a large extent, nutritionally essential and nearly exclusively derived from fish. Fish increase their membrane content by eating the phytoplankton rich in either the precursor alpha-linolenic acid or the more elongated compounds EPA and DHA. Fatty fish living in cold seas (e.g. mackerel, salmon and herring) are particularly rich in these compounds, which may give them a selective advantage in preventing low-temperature-related loss in membrane fluidity in cell membranes. Therefore, EPA and DHA may be considered nutritionally essential for most practical purposes and largely derived from fish and marine oils. [4]
This claim is further supported by epidemiological studies that show that fish consumption is inversely related to fatal coronary heart disease [17] and ischemic stroke [18]. That this benefit is derived primarily from consumption of EPA and DHA is also quite well established:
This evidence exists. Results of case-control studies, prospective cohort studies, and randomized controlled trials each indicate that modest consumption of fish or fish oil lowers the risk of cardiac mortality, specifically CHD death and sudden cardiac death. This effect appears to be nonlinear: compared with little or no intake, modest consumption (~250 mg/d) of the marine n-3 PUFA eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) significantly lowers risk of cardiac mortality, whereas higher intakes do not substantially further lower risk, suggesting a threshold of effect. The similarity of findings between observational studies of fish consumption and randomized controlled trials of n-3 PUFA supplementation suggests that, at least for cardiac mortality, much of the benefit of fish intake is related to the n-3 PUFA content. Consistent with this, when different types of fish meals are considered, lower risk is more strongly related to intake of fatty (oily or dark meat) fish, compared with lean (white meat) fish. The quantity of fish servings needed to consume an average of 250 mg/d EPA+DHA varies depending on the particular fish species, but for fatty fish (e.g., anchovies, herring, salmon, sardines, trout, white tuna) is ~1–2 servings/week.
The strength and consistency of the evidence, and the magnitude of the benefit, for lowering of cardiac mortality by fish consumption are each notable. The risk reduction is supported by consistent evidence from experimental studies and randomized trials investigating effects of fish or fish oil consumption on cardiovascular risk factors; case-control studies evaluating fish consumption or objective biomarkers of n-3 PUFA intake and risk of cardiac outcomes; prospective studies of habitual fish consumption and cardiac outcomes that have followed hundreds of thousands of people for many years across a range of countries; and randomized controlled trials of fish or fish oil consumption that have enrolled thousands of subjects and demonstrated reductions in clinical events. The magnitude of the benefit is also considerable: pooling of the prospective studies and controlled trials indicates that, compared with no intake, modest consumption (~250 mg/day [2¼ calories/day] of EPA+DHA, equivalent to ~1–2 servings/week of fatty fish) lowers risk of CHD mortality by 36%. Analyses restricted to populations free of established heart diease (i.e., primary prevention) demonstrate similar results. Fish intake may also reduce the risk of other cardiovascular and noncardiovascular outcomes, including but not limited to nonfatal heart attacks, ischemic stroke, atrial fibrillation, cognitive decline, and depression, but the evidence for these benefits is not yet as robust as for CHD death. [19].
There is some concern that the cardiovascular benefits of eating fish may be reduced by the danger of consuming toxic mercury compounds that are known to be present in fish that swim in our polluted waters (i.e. all of them). This area has not yet been well researched but current evidence suggests that the benefits of eating one or two servings of fatty fish per week far outweigh any risks from mercury poisoning [19].
The apparent benefits of consuming long-chain ω-3 fatty acids (i.e. fatty acids that are synthesisable from αLNA) have prompted a lot of research. It is fairly well established that although EPA and DHA can be synthesised from αLNA, such synthesis does not appear to be enough to reach optimal levels in humans. Conversion from αLNA to EPA does occur but it is limited in men and further conversion to DHA is very low. More conversion occurs in women, which may be due to a regulatory effect of oestrogen [20].
Apparently, some strains of algae also contain EPA and DHA, and so would be a good alternative to fish for vegetarians, but I cannot find any freely available journal articles to back up this claim. The idea appears to be that the fish get their EPA and DHA from algae in the first place, so we ought to be able to skip the fish-eating step and just get our long-chain ω-3 FAs straight from the algae. This sounds plausible, assuming humans have the ability to digest algae efficiently. I have found many references to algal sources of EPA and DHA but so far they have all either been in closed journals that require a subscription fee to read, or they have been marketing screeds for companies selling nutritional supplements to vegetarians. The only reference in a reputable, open journal that I have found is in the midst of an article about DHA in breast milk. Apparently they used algae-derived DHA as a nutritional supplement [21]. However, since I have found so many references to this claim, including some that seem quite reputable [22], I think it is probably true.
Less research has been performed to investigate the synthesisability of long-chain ω-6 fatty acids (i.e. those that are synthesisable from LA). However, it does seem that vegetarians have a lower level of arachidonic acid (AA) in their blood than omnivores [23]. There is some evidence to suggest that this is a deficiency caused by their inability to synthesise enough AA from the ω-6 fatty acids present in a vegetarian diet, whereas omnivores consume preformed AA in animal products, but this evidence is far from conclusive and other studies have produced varying results. I haven't found a meta-analysis of this research yet.
1.5.4 Animal Fats vs Vegetable Fats
Animal fats contain long-chain EFAs that are not found in any vegetable fats [4] [20] [23]. Apart from this, I have found no evidence to suggest any difference in health benefits or detriments between animal and vegetable fats.
1.6 Recommendations
Avoid trans fats. Do not consume any processed fats such as margarine or other partially hydrogenated fats. Beware of fried food served by restaurants, especially fast-food restaurants, that may use trans fats for frying.
Do not cook with polyunsaturated fats. Use saturated or monounsaturated fats for cooking, especially frying. All naturally occurring fats contain a mixture of saturated, polyunsaturated and monounsaturated fats. However, coconut fat is notable for being 92% saturated, far more than any other natural fat, and the rest of it is mostly (6%) monounsaturated.
Dairy products, such as milk and butter, come next with only 3-4% polyunsaturated fat. Thus, in the absence of coconut fat, butter is the next best fat for cooking. Beef fat is also only 3% polyunsaturated.
Consume some polyunsaturated vegetable oil to get the linoleic acid you need to synthesise ω-6 essential fatty acids - just don't cook with it. Herein lies the probable benefit of a "Mediterranean style" diet. This is especially important if you are a vegetarian and therefore do not consume any preformed long-chain ω-6 EFAs.
Consume plenty of green leafy plants to get the α-linolenic acid in the chloroplasts. Again, this is especially important if you are vegetarian and therefore must synthesise all your long-chain ω-3 EFAs yourself.
In order to ensure that you ingest a high ratio of ω-3 to ω-6 EFAs, worry about green leafy plants more than you do about vegetable oils. Flax is also a good source of ω-3 EFAs.
Consume one or two servings of fatty fish (e.g. salmon, herring or mackerel) per week for the EPA and DHA. Vegetarians should consider consuming algae such as Chlorella vulgaris or perhaps Spirulina plantensis as an alternative to fatty fish.
2 Protein
Proteins consist of amino acids connected together into long chains. An amino acid consists of a carbon atom bonded to: an amine group (a nitrogen atom bonded to two hydrogen atoms); a carboxyl group (a carbon atom bonded to a hydroxide group and double bonded to an oxygen atom); a hydrogen atom; and finally a side chain. Different amino acids have different side chains, which can vary from a single hydrogen atom to complex cyclic structures.
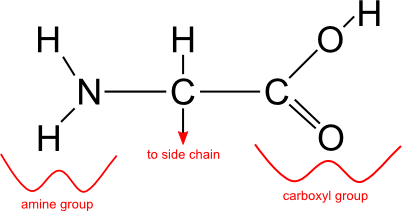
Amino acid
Proteins are formed by chaining together amino acids with peptide bonds.
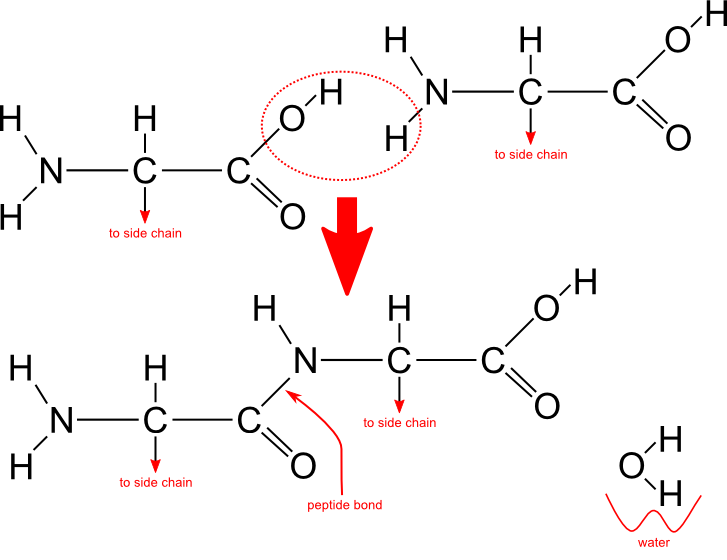
Peptide bond formation
The different amino acid side chains cause the proteins to have different shapes and functions.
2.1 Functions of Protein
Proteins are involved in pretty much every biological process. We are, to a large extent, made of proteins. There are more than 100,000 different proteins in the human body, making up everything from our body tissue, bones and hair to the chemical enzymes underlying our metabolism and the neurotransmitters in our nervous system. Proteins make up approximately 75% of the dry weight of a human body [28].
2.2 DNA
DNA consists of two long chains of relatively simple units called nucelotides. There are four different types of nucleotide: adenine (A), thymine (T), guanine (G) and cytosine (C). Thus a strand of DNA is a long sequence of A, T, G and C nucleotides. Each group of three nucleotides, called a codon, represents one amino acid. So a strand of DNA is really a representation of a long list of amino acids. A gene is a sequence of DNA that represents one or more protein sequences, made up of sequences of amino acids, each represented by a codon.
Since there are 4 types of nucleotide (A, T, G and C) and a codon is a sequence of 3 nucleotides, DNA can theoretically represent 43 = 64 different amino acids. However, in practice there are only 20 amino acids represented by the genetic code, most of which are represented by more than one codon. There are also three stop codons, which represent the end of a coding region.
| Amino Acid | Codon(s) |
|---|---|
| Arginine | CGT, CGC, CGA, CGG, AGA, AGG |
| Histidine | CAT, CAC |
| Lysine | AAA, AAG |
| Aspartate | GAT, GAC |
| Glutamate | GAA, GAG |
| Serine | TCT, TCC, TCA, TCG, AGT, AGC |
| Threonine | ACT, ACA, ACC, ACG |
| Asparagine | AAT, AAC |
| Glutamine | CAA, CAG |
| Cysteine | TGT, TGC |
| Glycine | GGT, GGC, GGA, GGG |
| Proline | CCT, CCC, CCA, CCG |
| Alanine | GCT, GCC, GCA, GCG |
| Isoleucine | ATT, ATC, ATA |
| Leucine | TTA, TTG, CTT, CTC, CTA, CTG |
| Methionine | ATG |
| Phenylalanine | TTT, TTC |
| Tryptophan | TGG |
| Tyrosine | TAC, TAT |
| Valine | GTT, GTC, GTA, GTG |
| Stop Codons | TAG, TGA, TAA |
2.3 Proteinogenic Amino Acids
Those amino acids that are used by standard cellular machinery to create proteins are known as proteinogenic. They are bound together with peptide bonds (see above) to form polypeptides, the sub-units of proteins. This process is part of the overall process of gene expression, i.e. the process by which the genetic code stored in DNA is translated into sequences of proteins.
As described above, there are 20 amino acids directly represented by the genetic code. However, in addition to those 20, there are two more amino acids which are indirectly represented by the genetic code and which are incorporated into proteins by cellular machinery in a unique manner: selenocysteine and pyrrolysine. The latter is found only in archaea and bacteria, never in eukaryotes such as humans.
There are therefore 22 proteinogenic amino acids, of which 21 are relevant to humans.
Many more amino acids are found in living organisms (hundreds, in fact) but the others are not considered proteinogenic either because they are not found in proteins at all or because they are not created directly by standard cellular machinery but through some other indirect method, such as enzyme activity on already extant proteins [24].
The phrase standard amino acids is sometimes used to refer to the 20 amino acids directly represented by the genetic code. However, one or both of selenocysteine and pyrrolysine are sometimes also included in the "standard" list. In this document, I shall use "standard amino acids" to refer to the 20 amino acids directly represented by the genetic code. Selenocysteine is a special case and pyrrolysine is irrelevant to human nutrition.
2.4 Essential Amino Acids
Plants are able to synthesise all of the standard amino acids. In contrast, animals are not. Animals must therefore consume amino acids in their diet in order to acquire those amino acids that they are incapable of synthesising.
Of the 20 standard amino acids, an adult human is capable of synthesising 12. The remaining 8 amino acids, which cannot be synthesised and therefore must be ingested, are known as essential amino acids. However, of the 12 synthesisable amino acids, 8 are known as conditionally essential because in certain developmental, dietary or disease conditions they cannot be sufficiently synthesised and so become effectively essential [25] [26] [27].
| Amino Acid | Essentiality |
|---|---|
| Isoleucine | Essential |
| Leucine | Essential |
| Lysine | Essential |
| Methionine | Essential |
| Phenylalanine | Essential |
| Threonine | Essential |
| Tryptophan | Essential |
| Valine | Essential |
| Histidine | Essential for infants and in case of kidney failure, non-essential for healthy adults |
| Tyrosine | Essential for infants and in case of kidney failure, non-essential for healthy adults |
| Arginine | Essential for infants, non-essential for adults |
| Cysteine | Essential for infants and in case of trauma or infection, non-essential for healthy adults |
| Glutamine | Essential after major injury, operations, burns, infections, non-essential for healthy adults |
| Glycine | Essential for infants, non-essential for healthy adults |
| Proline | Essential after burns, non-essential for healthy adults |
| Serine | Essential in case of kidney failure, non-essential for healthy adults |
| Asparagine | Non-essential |
| Aspartate | Non-essential |
| Glutamate | Non-essential |
| Alanine | Non-essential |
However, even though non-essential amino acids can be synthesised by the human body, doing so still requires the presence of sufficient quantities of their precursor molecules. Thus different amino acids may compete for limited resources for their synthesis, effectively becoming limiting metabolic factors even though they are theoretically non-essential [25]. It is therefore important to consume a good balance of proteinogenic amino acids, including non-essential amino acids, but with particular regard to essential ones.
2.5 Sources of Essential Amino Acids
Foods that not only contain all the amino acids essential for humans but do so in appropriate proportions are known as complete proteins. Animal products, such as meat and dairy, are complete proteins [29].
There are, as far as I know, only two vegetarian complete proteins: soybeans and quinoa [30]. The Food and Agriculture Organization of the United Nations (FAO) has produced a recommended profile of amino acids essential to human nutrition, which is here compared with quinoa, soybeans and wheat [30]:
| Amino Acid | Quinoa | Wheat | Soybean | FAO |
|---|---|---|---|---|
| Isoleucine | 4.0 | 3.8 | 4.7 | 4.0 |
| Leucine | 6.8 | 6.6 | 7.0 | 7.0 |
| Lysine | 5.1 | 2.5 | 6.3 | 5.5 |
| Phenylalanine plus Tyrosine | 8.4 | 7.5 | 8.2 | 6.0 |
| Cysteine plus Methionine | 4.6 | 3.9 | 2.8 | 3.5 |
| Threonine | 3.7 | 2.9 | 3.9 | 4.0 |
| Tryptophan | 1.2 | 1.3 | 1.2 | 1.0 |
| Valine | 4.8 | 4.7 | 4.9 | 5.0 |
You can see in the above table that both quinoa and soybean meet (or very nearly meet) the FAO recommendations for all the essential amino acids. Wheat also comes close but is deficient in lysine. Cereals, nuts, seeds and many fruits and vegetables are also deficient in lysine. But legumes - lentils and beans - have sufficient lysine but are deficient in cysteine and methionine instead. Thus it is possible for vegetarians to consume adequate amounts of all essential amino acids as long as they take care to combine complementary sources of proteins [31].
2.6 Recommendations
Consuming complete proteins is the easiest way to ensure that you get a full complement of essential amino acids in your diet. Animal products, including milk and eggs, contain everything you need in a form readily digestible by humans. Quinoa and soybeans are good alternatives for vegetarians.
Vegetarians - especially vegans who do not eat eggs or dairy - should take care to eat a varied diet. Combine rice or cereals with beans or lentils to get a balanced mixture of all the essential amino acids.
Variety seems to be the key: it is not necessary to carefully compose every meal, just make sure your diet is varied.
3 Carbohydrates
Carbohydrates are molecules composed of carbon, hydrogen and oxygen, with the hydrogen and oxygen in a 2:1 ratio. They are also known as saccharides.
3.1 Monosaccharides
Natural carbohydrates are usually built from simple carbohydrates known as monosaccharides. A monosaccharide usually consists of a chain of carbon atoms, one of which is double bonded to an oxygen atom (this is called a carbonyl group) and many of which are bonded to an oxygen atom which is bonded to a hydrogen atom (these are called hydroxyl groups).
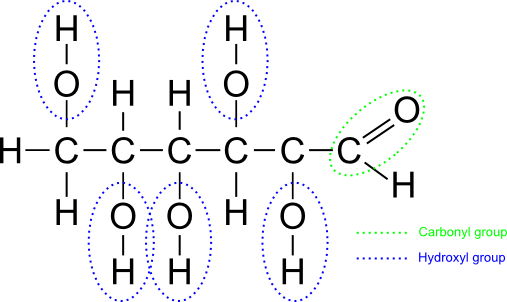
A monosaccharide (glucose)
Monosaccharides often exist in more than one form. For example, an open-chain form such as the one pictured above and also a cyclic form in which the carboxyl group is bonded to one of the hydroxyl groups.
| [1] | 2008. From Stargazers to Starships. David P. Stern. An online book published by NASA. Chapter 15: Energy. Available at: http://www-istp.gsfc.nasa.gov/stargaze/Senergy.htm |
| [2] | 2008. Fat-Soluble Vitamins. J. Anderson and L. Young. A fact sheet produced by Colorado State University, which provides a list of references for its claims. Available at: http://www.ext.colostate.edu/pubs/foodnut/09315.html |
| [3] | 1932. On The Fatty Acids Essential in Nutrition III. George O. Burr, Mildred M. Burr and Elmer S. Miller. The Journal of Biological Chemistry, Vol. XCVII, No. 1. Available at: http://www.jbc.org/cgi/reprint/97/1/1.pdf |
| [4] | (1, 2, 3, 4) 2001. n-3 Fatty acids and the inflammatory response — biological background. R. De Caterina and G. Basta. European Heart Journal Supplements, 3 (Supplement D). Available at: http://eurheartjsupp.oxfordjournals.org/cgi/reprint/3/suppl_D/D42.pdf |
| [5] | 1980. Epidemiological studies in the Upernavik District, Greenland. N. Kromann and A. Green. Acta Medica Scandinavica, 208(5):401-6. Abstract available at: http://www.ncbi.nlm.nih.gov/pubmed/7457208 |
| [6] | 2000. Arachidonic Acid. Daniele Piomelli. Neuropsychopharmacology: The Fifth Generation of Progress. A collection of papers produced by the American College of Neuropsychoparmacology. Available at: http://www.acnp.org/g4/GN401000059/Default.htm |
| [7] | 2008. Arachidonic acid and the brain. S. Rapoport. The Journal of Nutrition 138: 2515-2520. Available at: http://jn.nutrition.org/cgi/content/full/138/12/2515 |
| [8] | 2010. Meta-analysis of prospective cohort studies evaluating the association of saturated fat with cardiovascular disease. P. W. Siri-Tarino, Q. Sun, F. B. Hu and R. M. Krauss. American Journal of Clinical Nutrition, 91(3): 535-546. Abstract available at: http://www.ajcn.org/cgi/content/abstract/91/3/535 |
| [9] | 2009. A Systematic Review of the Evidence Supporting a Causal Link Between Dietary Factors and Coronary Heart Disease. A. Mente, L. de Koning, H. S. Shannon and S. S. Anand. Archives of Internal Medicine, Vol. 169, No. 7. Available at: http://archinte.ama-assn.org/cgi/content/full/169/7/659 |
| [10] | 2010. Saturated fat. Part of the "Eat well, be well" online guide to a healthy diet. Available at: http://www.eatwell.gov.uk/healthydiet/fss/fats/satfat/ |
| [11] | 1981. Cholesterol, coconuts, and diet on Polynesian atolls: a natural experiment: the Pukapuka and Tokelau island studies. I. A. Prior, F. Davidson, C. E. Salmond and Z. Czochanska. American Journal of Clinical Nutrition, Vol. 34, 1552-1561. Available at: http://www.ajcn.org/cgi/reprint/34/8/1552 |
| [12] | 2004. Dietary fats, carbohydrate, and progression of coronary atherosclerosis in postmenopausal women. D. Mozaffarian, Eric B. Rimm and David M Herrington. American Journal of Clinical Nutrition, Vol. 80, No. 5, 1175-1184. Available at: http://www.ajcn.org/cgi/content/full/80/5/1175 |
| [13] | 2001. Health effects of oxidized heated oils. M. Grootveld, C. J. L. Silwood, P. Addis, A. Claxson, B. Bonet Serra and M. Viana. Foodservice Research International, Vol. 13, No. 1, 41-55. Abstract available at: http://www3.interscience.wiley.com/journal/118986429/abstract |
| [14] | (1, 2) 1997. Health effects of trans fatty acids. A. Ascherio and W. C. Willet. American Journal of Clinical Nutrition, Vol. 66, 1006S-1010S. Available at: http://www.ajcn.org/cgi/reprint/66/4/1006S |
| [15] | 2008. Lipoprotein Management in Patients With Cardiometabolic Risk: Consensus statement from the American Diabetes Association and the American College of Cardiology Foundation. J. D. Brunzell, M. Davidson, C. D. Furberg, R. B. Goldberg, B. V. Howard, J. H. Stein and J. L. Witztum. Diabetes Care, Vol. 31, No. 4, 811-822. Available at: http://care.diabetesjournals.org/content/31/4/811.long |
| [16] | 2006. TRANSforming the Food Supply. The final report of the Trans Fat Task Force, co-chaired by Health Canada and the Heart and Stroke Foundation of Canada. Available at: http://www.hc-sc.gc.ca/fn-an/nutrition/gras-trans-fats/tf-ge/tf-gt_rep-rap-eng.php |
| [17] | 2004. Accumulated evidence on fish consumption and coronary heart disease mortality: a meta-analysis of cohort studies. K. He, Y. Song, M. L. Daviglus, K. Liu, L. Van Horn, A. R. Dyer and P. Greenland. Circulation, Vol. 109, No. 22, 2705-2711. Available at: http://circ.ahajournals.org/cgi/content/full/109/22/2705 |
| [18] | 2004. Fish consumption and incidence of stroke: a meta-analysis of cohort studies. K. He, Y. Song, M. L. Daviglus, K. Liu, L. Van Horn, A. R. Dyer, U. Goldbourt and P. Greenland. Stroke, Vol. 35, No. 7, 1538-1542. Available at: http://stroke.ahajournals.org/cgi/content/full/35/7/1538 |
| [19] | (1, 2) 2009. Fish, Mercury, Selenium and Cardiovascular Risk: Current Evidence and Unanswered Questions. D. Mozaffarian. International Journal of Environmental Research and Public Health, Vol. 6, 1894-1916. Available at: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2705224/ |
| [20] | (1, 2) 2005. Conversion of α-linolenic acid to longer-chain polyunsaturated fatty acids in human adults. Graham C. Burdge and Philip C. Calder. Reproduction Nutrition Development, vol. 45, No. 5. Available at: http://rnd.edpsciences.org/articles/rnd/pdf/2005/05/r5505.pdf |
| [21] | 2000. Effect of docosahexaenoic acid supplementation of lactating women on the fatty acid composition of breast milk lipids and maternal and infant plasma phospholipids. C. L. Jensen, M. Maude, R. E. Anderson and W. C. Heird. The American Journal of Clinical Nutrition, Vol. 71, No. 1, 292S-299s. Available at: http://www.ajcn.org/cgi/content/full/71/1/292S |
| [22] | 2006. Biomass Nutrient Profiles of Three Microalgae: Spirulina platensis, Chlorella vulgaris, and Isochrisis galbana. Ö. Tokuşoglu and M. K. Üunal. Journal of Food Science, Vol. 68, Issue 4, 1144-1148. Abstract available at: http://www3.interscience.wiley.com/journal/118832357/abstract |
| [23] | (1, 2) 1990. Reduced arachidonate in serum phospholipids and cholesteryl esters associated with vegetarian diets in humans S. D. Phinney, R. S. Odin, S. B. Johnson and R. T. Holman. The American Journal of Clinical Nutrition, Vol. 51, No. 3, 385-392. Available at: http://www.ajcn.org/cgi/reprint/51/3/385 |
| [24] | 2007. Natural expansion of the genetic code. A. Ambrogelly, S. Palioura and D. Söll. Nature Chemical Biology, Vol. 3, 29-35. Abstract available at: http://www.nature.com/nchembio/journal/v3/n1/abs/nchembio847.html |
| [25] | (1, 2) 2000. Dispensable and Indispensable Amino Acids for Humans. P. J. Reeds. The Journal of Nutrition, Vol. 130, No. 7, 1835S-1840S. Available at: http://jn.nutrition.org/cgi/content/full/130/7/1835S |
| [26] | 2004. What Are the Essential Elements Needed for the Determination of Amino Acid Requirements in Humans?. P. Fürst and P. Stehle. The Journal of Nutrition, Vol. 134, No. 6, 1558S-1565. Available at: http://jn.nutrition.org/cgi/content/full/134/6/1558S |
| [27] | 2004. Arginine deficiency in preterm infants: biochemical mechanisms and nutritional implications. G. Wu, L. A. Jaeger, F. W. Bazer and J. M. Rhoads. The Journal of Nutritional Biochemistry, Vol. 15, Issue 8, 442-451. Abstract available at: http://www.jnutbio.com/article/S0955-2863%2804%2900070-1/abstract |
| [28] | 1993. Introduction to Physical Science. J. Shipman, J. Wilson and A. Todd. Chapter 15. D. C. Heath. |
| [29] | 2003. Sustainability of meat-based and plant-based diets and the environment. D. Pimentel and M. Pimentel. The American Journal of Clinical Nutrition, Vol. 78, No. 3, 660S-663S. Available at: http://www.ajcn.org/cgi/content/full/78/3/660S |
| [30] | (1, 2) 1993. Quinoa: An Emerging "New" Crop with Potential for CELSS. G. Schlick and D. L. Bubenheim. NASA Technical Paper 3244. Available at: http://ntrs.nasa.gov/archive/nasa/casi.ntrs.nasa.gov/19940015664_1994015664.pdf |
| [31] | 1994. Plant proteins in relation to human protein and amino acid nutrition. V. R. Young and P. L. Pellett. The American Journal of Clinical Nutrition, Vol. 59, No. 5, 1203S-1212S. Available at: http://www.ajcn.org/cgi/reprint/59/5/1203S |